Vertebral Endplates
are a Significant Source of Chronic Low Back Pain
Research Findings:
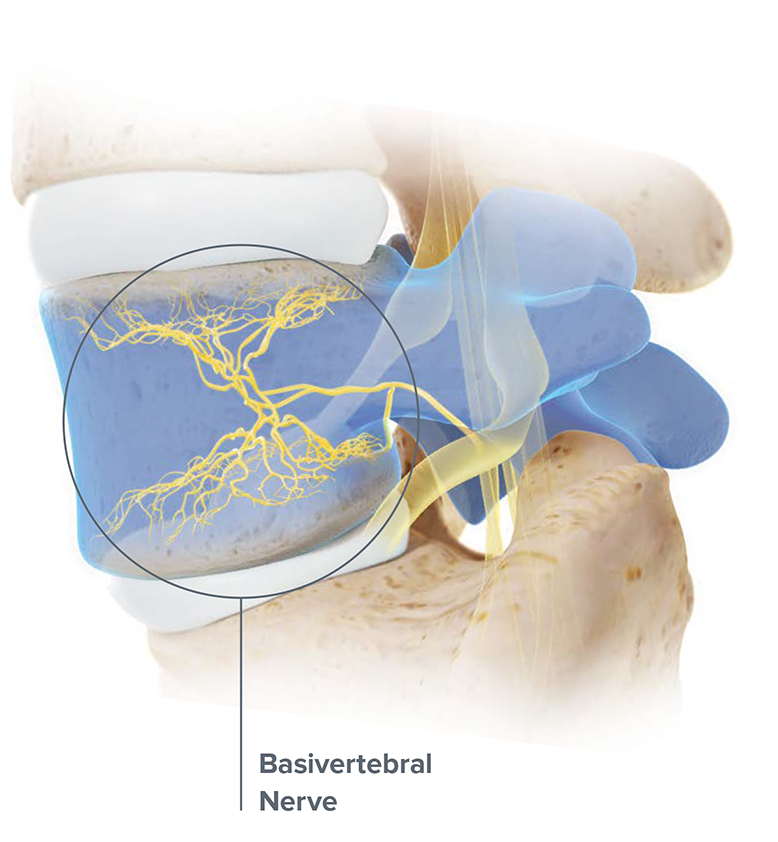
Collectively, these findings validate vertebral endplates as a significant source of chronic low back pain in patients with Type 1 or Type 2 modic changes, also referred to as vertebrogenic pain, and this pain is transmitted via the basivertebral nerve.
1. Vertebral endplates are more innervated than intervertebral discs1
2. The basivertebral nerve innervates the endplates and proliferates in damaged and degenerated endplates2,3
3. Modic changes and associated endplate damage strongly correlate with chronic low back pain4,5,6,7,8
REFERENCES
1. Fields AJ, Liebenberg EC, Lotz JC. Innervation of pathologies in the lumbar vertebral endplate and intervertebral disc. The Spine Journal: Official Journal of the North American Spine Society 2014;14(3):513-521.
2. Bailey JF, Liebenberg E, Degmetich S, Lotz JC. Innervation patterns of PGP 9.5-positive nerve fibers within the human lumbar vertebra. Journal of Anatomy 2011;218(3):263-70.
3. Lotz JC, Fields AJ, Liebenberg EC. The Role of the Vertebral End Plate in Low Back Pain. Global Spine J 2013;03:153-64.
4. Modic MT, Steinberg PM, Ross JS, Masaryk TJ, Carter JR. Degenerative disk disease: assessment of changes in vertebral body marrow with MR imaging. Radiology 1988;166:193-9.
5. Carragee EJ, Alamin TF, Miller JL, Carragee JM. Discographic, MRI and psychosocial determinants of low back pain disability and remission: a prospective study in subjects with benign persistent back pain. The Spine Journal: Official Journal of the North American Spine Society 2005;5(1):24-35.
6. Weishaupt D, Zanetti M, Hodler J, et al. Painful Lumbar Disk Derangement: Relevance of Endplate Abnormalities at MR Imaging. Radiology 2001;218(2):420-7.
7. Kuisma M, Karppinen J, Niinimaki J, et al. Modic changes in endplates of lumbar vertebral bodies: prevalence & association with low back and sciatic pain among middle-aged male workers. Spine 2007;32(10):1116-22.
8. Mok K, Samartzis D, Karppinen J, et al. Modic changes of the lumbar spine: prevalence, risk factors, and association with disc degeneration and low back pain in a large-scale population-based cohort. The Spine Journal: Official Journal of the North American Spine Society 2016;16(1):32-41.
The Intracept Procedure
for the Relief of Chronic Vertebrogenic Low Back Pain
The Intracept Procedure is a minimally invasive procedure targeting the basivertebral nerve for the relief of chronic vertebrogenic low back pain.
Key Benefits of Intracept:
• Provides a treatment option for patients who have not responded to conservative therapy
• Minimally invasive, outpatient procedure
• Implant-free and preserves the structure of the spine
• Provides durable relief of chronic vertebrogenic low back pain

Intracept Procedure Steps

1. Access the pedicle
Under fluoroscopic guidance, the Intracept Introducer Cannula is advanced through the pedicle
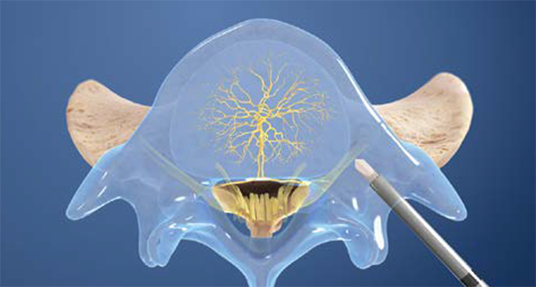

2. Create the channel
The Intracept Curved Cannula is utilized to create a channel to the trunk of the basivertebral nerve
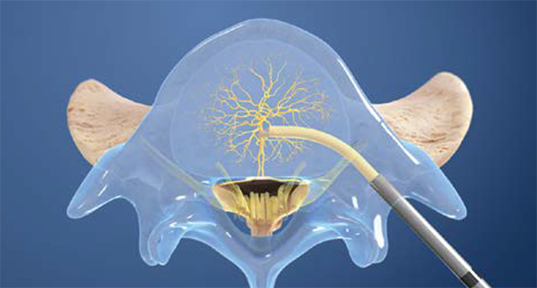

3. Place the RF Probe
The Intracept Radiofrequency Probe is inserted into the curved path and placed at the basivertebral nerve


4. Ablate the BVN
The Relievant Radiofrequency Generator is utilized to ablate the basivertebral nerve

The Intracept Procedure Indications
• Chronic low back pain of at least 6 months duration; and
• Failure to respond to at least 6 months of conservative care; and
• MRI demonstrated Modic Type 1 or Type 2 changes at one or more vertebrae from L3 to S1 documented by at least one of the following:
– Modic Type 1 and/or Modic Type 2 – Endplate changes, inflammation, edema, disruption, and/or fissuring
– Fibrovascular bone marrow changes (hypointensive signal for Modic Type 1)
– Fatty bone marrow replacement (hyperintensive signal for Modic Type 2)
Indicatons for Use: The Intracept Intraosseous Nerve Ablation System is intended to be used in conjunction with radiofrequency (RF) generators for the ablation of basivertebral nerves of the L3 through S1 vertebrae for the relief of chronic low back pain of at least six months duration that has not responded to at least six months of conservative care, and is also accompanied by features consistent with Type 1 or Type 2 Modic changes on an MRI such as inflammation, edema, vertebral endplate changes, disruption and fissuring of the endplate, vascularized fibrous tissues within the adjacent marrow, hypointensive signals (Type 1 Modic change), and changes to the vertebral body marrow including replacement of normal bone marrow by fat, and hyperintensive signals (Type 2 Modic change).

Doctor Discussion Guide
Not sure if this procedure will work for you?
Review this guide and Talk with us during your visit using this guide.

